BMI for Children and Teens: Complete Healthy Weight Guide by Age

Understanding BMI in Children and Teens
Body Mass Index (BMI) is a widely used indicator to evaluate whether a child is growing within a healthy weight range. During childhood and adolescence, the body develops rapidly, and weight must be assessed in relation to height, age, and gender. BMI provides a structured way to track this development over time.
Unlike adults, children require BMI interpretation through percentiles, which compare them to peers of the same age and sex. This approach helps identify early signs of underweight or overweight conditions. Understanding BMI correctly supports better decisions about nutrition, activity, and overall health.
Key Points:
- BMI reflects weight relative to height
- Percentiles make BMI age-specific
- Helps monitor long-term growth trends
- Useful for early health risk detection
What is BMI and How is it Calculated
BMI is calculated using a simple formula that relates body weight to height. Although the calculation is easy, its interpretation in children requires additional context. The BMI value alone does not define health but acts as a screening tool when combined with growth data.
Tracking BMI regularly allows parents and healthcare providers to observe patterns rather than relying on a single measurement. This makes it more effective in identifying gradual changes in weight and growth. Consistency in tracking is more valuable than isolated results.
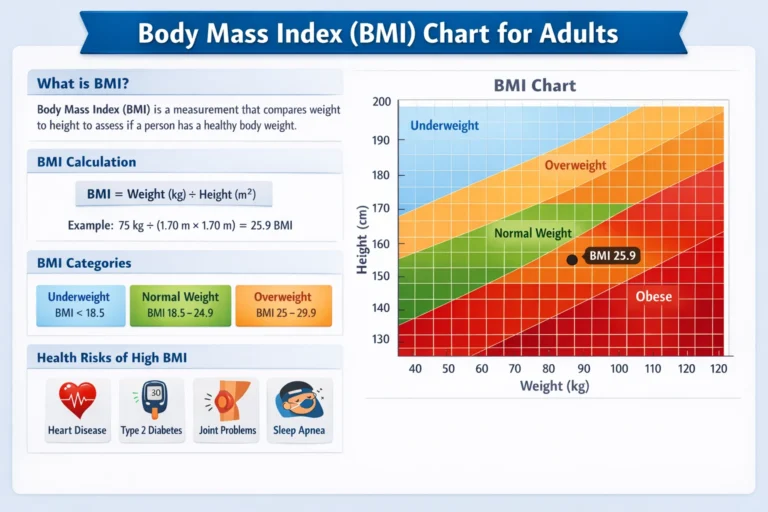
BMI Formula
BMI = Weight (kg) ÷ Height (m²)
Important Notes:
- Simple and quick calculation method
- Does not directly measure body fat
- Works best when tracked over time
- Requires percentile charts for accuracy
Why BMI is Different for Children
Children are constantly growing, and their body composition changes with age. This makes fixed BMI ranges unsuitable for accurate assessment. Instead, BMI must be evaluated based on developmental stages, which vary from early childhood to adolescence.
Gender differences also influence BMI, especially during puberty when hormonal changes affect fat and muscle distribution. These natural variations make percentile-based analysis essential. It ensures that BMI reflects real growth patterns rather than static numbers.
Factors That Influence BMI:
- Growth spurts and developmental stages
- Hormonal changes during puberty
- Differences in muscle and fat composition
- Individual growth variations
BMI Percentile Categories Explained
BMI percentiles classify children into weight categories based on comparison with standard growth charts. These categories provide a clearer understanding of whether a child’s weight is appropriate for their age and gender. They are essential for identifying potential health risks early.
Instead of focusing on a single number, percentiles show how a child compares with others. This makes them more reliable and clinically meaningful. Monitoring percentile trends over time gives a better picture of overall growth.
| Percentile Range | Category | Meaning |
|---|---|---|
| Below 5th | Underweight | Possible nutritional concern |
| 5th – 85th | Healthy Weight | Balanced growth |
| 85th – 95th | Overweight | Increased health risk |
| Above 95th | Obese | High risk of complications |
Key Insights:
- Percentiles are more important than BMI values
- Growth trends matter more than single readings
- Early detection improves health outcomes
Age-Based BMI Guide for Growth Stages
Ages 2–5 Years: Early Growth Phase
During early childhood, growth is rapid and often uneven. BMI may fluctuate due to changes in appetite and activity levels, which is generally normal. The focus should be on building a strong nutritional foundation and encouraging active play.
Children at this stage depend on caregivers for food and lifestyle habits. Establishing healthy routines early helps maintain stable growth patterns. Small, consistent habits have long-term benefits.
Focus Areas:
- Balanced and nutrient-rich meals
- Active play instead of screen time
- Limited sugary snacks and drinks
- Regular eating routines
Ages 6–12 Years: Habit Development Phase
This stage is crucial because children begin developing independent habits that influence their BMI. School routines, peer influence, and lifestyle choices start shaping their health behaviors. Monitoring BMI during this time helps prevent gradual weight issues.
Children may become less active and more exposed to processed foods. Encouraging physical activity and structured meals helps maintain balance. Healthy habits formed here often continue into adulthood.
Healthy Practices:
- Encourage sports and outdoor play
- Maintain consistent meal schedules
- Reduce junk food consumption
- Limit screen time
Ages 13–19 Years: Adolescent Growth Phase
Adolescence involves significant physical and emotional changes that affect BMI. Hormonal shifts, growth spurts, and lifestyle factors can cause noticeable weight changes. It is important to approach BMI with flexibility during this stage.
Teenagers may also face body image concerns, which can influence eating habits. A supportive environment helps them maintain healthy behaviors. Focus should remain on overall well-being rather than appearance.
Important Considerations:
- Encourage balanced nutrition
- Support regular physical activity
- Address emotional well-being
- Avoid extreme dieting habits
Healthy BMI Reference by Age
| Age Group | Typical BMI Range | Insight |
|---|---|---|
| 2–5 years | 14 – 17 | Natural fluctuations are normal |
| 6–12 years | 15 – 20 | Stable growth phase |
| 13–19 years | 18 – 24 | Influenced by puberty |
BMI ranges provide general guidance, but percentile charts offer more accurate evaluation. Tracking changes over time is more important than focusing on exact numbers. Consistency in growth patterns indicates healthy development.
Key Points:
- Use percentiles for accurate assessment
- BMI ranges are general guidelines
- Growth consistency matters most
- Regular monitoring is essential
Causes of Unhealthy BMI in Children
Unhealthy BMI in children is usually the result of multiple combined factors rather than a single cause. Lifestyle habits, diet, and environment all play a role in shaping weight patterns. Understanding these causes helps in creating effective solutions.
Modern lifestyles often reduce physical activity and increase access to unhealthy foods. These changes can gradually lead to weight imbalance. Addressing root causes is key to long-term improvement.
Common Causes:
- Poor diet and high sugar intake
- Lack of physical activity
- Excess screen time
- Genetic and environmental influences
Health Risks of Abnormal BMI
Both underweight and overweight conditions can affect a child’s physical and emotional health. Identifying these risks early allows for timely action and better outcomes. BMI helps highlight these concerns before they become serious.
Children with abnormal BMI may experience reduced energy, health complications, or emotional challenges. A balanced approach is needed to address both physical and mental well-being.
Underweight Risks:
- Weak immune system
- Delayed growth
- Nutritional deficiencies
Overweight Risks:
- Diabetes and heart disease
- High blood pressure
- Low self-confidence
Smarter health starts here—explore BMI guides made for you.
How to Maintain a Healthy BMI
Maintaining a healthy BMI requires consistent habits rather than short-term changes. A balanced lifestyle that includes proper nutrition, activity, and rest is essential for healthy growth. Small daily improvements can lead to long-term results.
Parents and caregivers play a key role in shaping these habits. Creating a supportive environment encourages children to adopt healthier behaviors naturally.
Effective Strategies:
- Provide balanced and nutritious meals
- Encourage daily physical activity
- Maintain proper sleep routines
- Limit screen time
Sleep and Its Impact on BMI
Sleep plays an important role in regulating metabolism and maintaining a healthy weight. Poor sleep can disrupt hormones that control hunger, leading to overeating and weight gain. Proper sleep supports both physical and mental development.
Children who get enough sleep are more likely to have better energy levels and healthier habits. Sleep should be considered a key part of weight management.
| Age Group | Recommended Sleep |
|---|---|
| 6–12 years | 9–12 hours |
| 13–18 years | 8–10 hours |
Why Sleep Matters:
- Regulates appetite hormones
- Supports growth and recovery
- Improves focus and energy
- Reduces risk of weight gain
When to Consult a Doctor
BMI is a useful screening tool, but certain situations require professional evaluation. Sudden or extreme changes in weight should not be ignored, as they may indicate underlying health issues. Early intervention can prevent long-term complications.
Parents should observe growth patterns and overall health rather than focusing only on numbers. Consulting a doctor ensures accurate diagnosis and guidance.
Consult a Doctor If:
- BMI is too high or too low
- Sudden weight changes occur
- Growth appears delayed
- Child feels weak or fatigued
FAQs
What is a healthy BMI for children?
A healthy BMI falls between the 5th and 85th percentile based on age and gender.
Is BMI accurate for children?
BMI is a screening tool and should be combined with overall health evaluation.
How often should BMI be checked?
It is recommended to check BMI once or twice a year during growth years.
What causes high BMI in children?
Poor diet, low activity levels, and excessive screen time are common causes.
Can children maintain a healthy BMI easily?
Yes, with consistent healthy habits and proper guidance from parents.
Conclusion
BMI is a valuable tool for understanding growth and identifying potential health risks in children and teens. However, it should always be used alongside a broader view of lifestyle, nutrition, and emotional health. A balanced approach ensures better long-term outcomes.
Focusing on healthy habits rather than numbers helps children grow confidently and sustainably. With proper support, children can achieve not just a healthy BMI but a healthier life overall.
Find out your BMI—simple, fast, and accurate.